ADHD in Children
Attention-deficit/hyperactivity disorder (ADHD) is a common neurodevelopmental condition characterised by three core symptoms: inattention, hyperactivity, and impulsivity. These symptoms can significantly affect a young person’s functioning at home, school, and in social settings.
However, ADHD rarely exists in isolation. Many children and adolescents with ADHD present with co-existing conditions, including conduct disorder, oppositional defiant disorder (ODD), anxiety disorders, and depressive disorders. Understanding this complexity is essential for accurate diagnosis and effective treatment planning.
The Importance of Effective Triage and Initial Assessment
Across many healthcare systems, waiting lists for ADHD assessments have grown significantly, sometimes extending to several years. Because of this, effective triage has become critical to ensure that young people are directed to the most appropriate clinician at the earliest opportunity.
Some services use structured screening tools such as the Development and Well-Being Assessment (DAWBA), while others have begun experimenting with artificial intelligence–assisted triage systems. These approaches can help prioritise cases and organise referrals more efficiently.
Nevertheless, a senior clinician with expertise in neurodevelopmental disorders can often be just as effective in triage decision-making. Skilled clinical judgement can help reduce duplication and ensure the correct pathway from the outset. For example, a child presenting with severe ADHD symptoms may benefit from being assessed directly by a prescriber, allowing timely initiation of stimulant medication when appropriate.
Santosh, P (2017) Stimulant medication to treat attention-deficit/hyperactivity disorder. BMJ; 358 doi: https://doi.org/10.1136/bmj.j2945
Service Configuration: Looking Beyond a Single Diagnosis
ADHD is frequently part of a broader cluster of neurodevelopmental and mental health conditions. It commonly co-occurs with:
Autism spectrum disorder (ASD)
Developmental coordination disorder (DCD)
Developmental language disorder (DLD)
Intellectual disability (ID)
Foetal alcohol spectrum disorder (FASD)
Other mental health conditions
Most individuals present with multiple, interrelated needs. However, healthcare pathways that focus narrowly on a single diagnosis risk overlooking other important conditions and support requirements.
This fragmented approach can lead to repeated and lengthy assessments, which can be both stressful for families and costly for healthcare systems such as the NHS. Integrated, multidisciplinary pathways are therefore essential to provide comprehensive and efficient care.
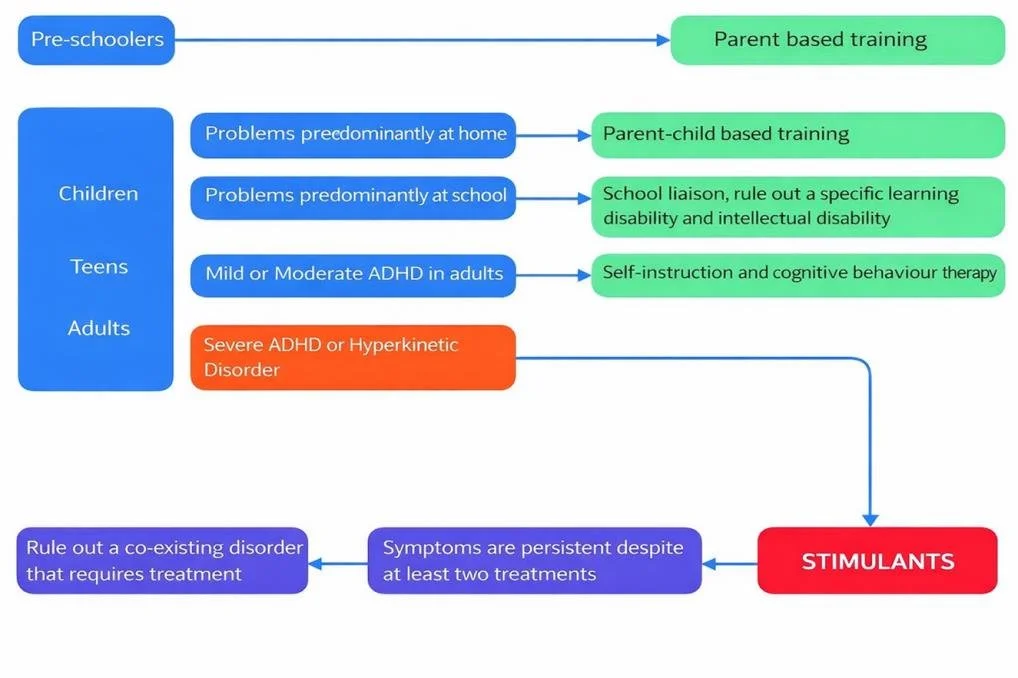
Treatment Approaches in ADHD
Treatment decisions in ADHD depend on symptom severity, functional impairment, and the presence of co-existing conditions.
Non-pharmacological interventions
In children and young people, non-pharmacological approaches are typically recommended as the first line of treatment. These may include:
Parent training programmes
Behavioural interventions
Psychological therapies
Educational support
These strategies aim to improve behaviour, coping strategies, and environmental support before medication is considered.
Pharmacological treatment
Medication becomes particularly important in certain situations.
Stimulant medication may be recommended when:
ADHD symptoms are severe, or
Non-pharmacological approaches have not been effective.
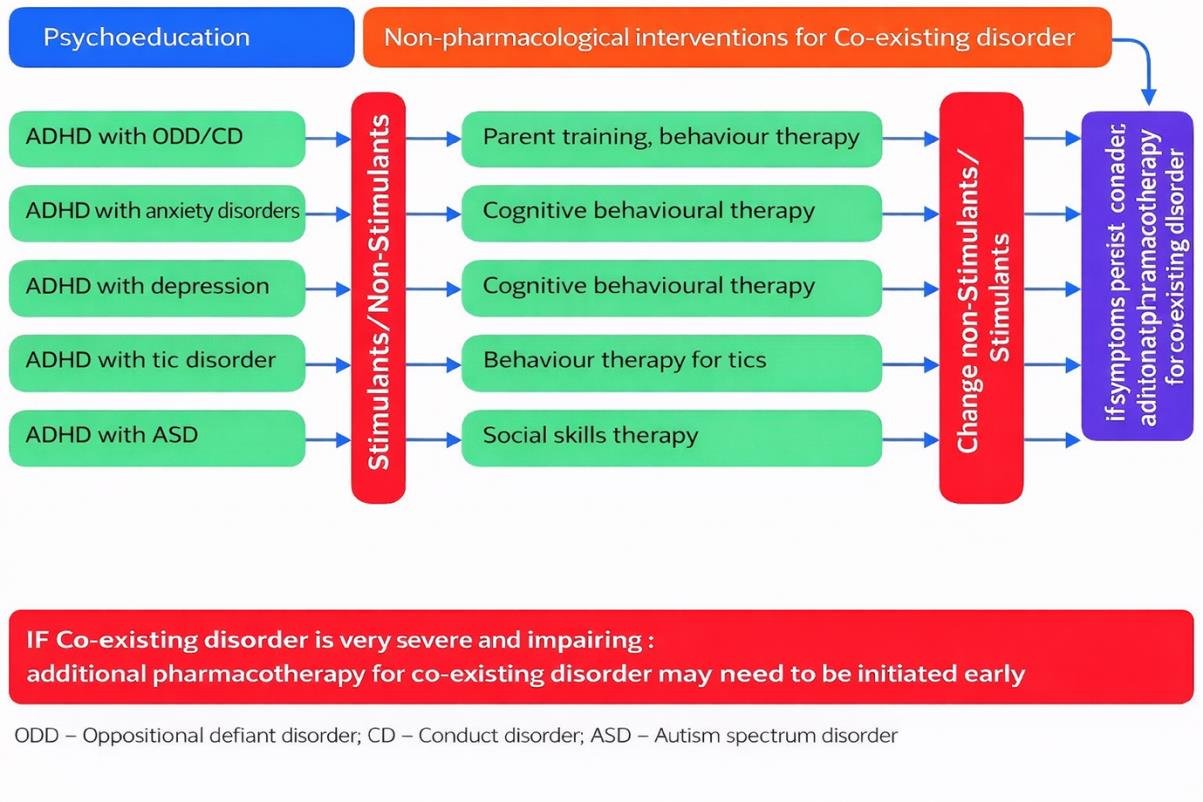
Importantly, stimulant medications can still be used in individuals who have ADHD alongside many co-existing conditions, including:
Anxiety disorders
Oppositional defiant disorder
Conduct disorder
Tic disorders
Autism spectrum disorder
Santosh, P (2017) Stimulant medication to treat attention-deficit/hyperactivity disorder. BMJ; 358 doi: https://doi.org/10.1136/bmj.j2945
NICE Guidance on ADHD Treatment
According to the UK National Institute for Health and Care Excellence (NICE) guidelines, medication should not be used in isolation. Instead, drug treatment should form part of a comprehensive care plan that includes:
Psychological interventions
Behavioural strategies
Educational support and advice
This multimodal approach ensures that both the symptoms of ADHD and the broader developmental needs of the young person are addressed.
Looking to the Future: Monitoring and Service Transitions
As ADHD care evolves, several developments are shaping future service delivery.
Remote monitoring
When medication is prescribed, regular monitoring is required. Increasingly, this can be conducted remotely using ambulatory or personal monitoring devices, after appropriate instruction is given to parents or caregivers.
Improving transitions between services
Transitions between services — such as:
Child to adolescent services
Adolescent to adult services
Private care to NHS services
— can sometimes be complicated and disruptive.
However, with clear criteria and well-designed pathways, these transitions do not need to become bureaucratic obstacles. When services collaborate effectively, transitions can support continuity of care and prevent breakdowns in treatment.
Ultimately, the goal should always be to ensure that young people receive consistent, coordinated support throughout their developmental journey.
First published on medium: https://medium.com/p/e612e77214dc